Bellerose, Delphine
(2011)
Benzodiazepine use in Ireland.
Drugnet Ireland,
Issue 36, Winter 2010,
pp. 1-3.
The latest addition to the HRB Trends Series, Problem benzodiazepine use in Ireland: treatment (2003 to 2008) and deaths (1998 to 2007),1 was published in December 2010. The paper describes treated problem benzodiazepine use as recorded by the National Drug Treatment Reporting System (NDTRS) for the years 2003–2008, and poisoning deaths where a benzodiazepine was implicated as recorded by the National Drug-Related Deaths Index (NDRDI) for the years 1998–2007. This is the first time that data from the NDTRS and the NDRDI have been presented together in a Trends Series paper, providing a more complete picture of problem benzodiazepine use and its consequences. The main findings are summarised below.
Numbers treated and number of deaths
In the period 2003–2008 the annual number of treated cases reporting a benzodiazepine as a problem substance increased by just over 63%, rising from 1,054 in 2003 to 1,719 in 2008 (Table 1). The number of cases who reported a benzodiazepine as their main problem substance was relatively small, but increased by 120%, from 76 in 2003 to 167 in 2008. The number of cases who reported a benzodiazepine as an additional problem substance was much larger, and increased by 59%, from 982 in 2003 to 1,562 in 2008. These increases may be explained by a combination of factors: an increase in the number of treatment places, an increase in problem benzodiazepine use among the population and an increase in reporting to the NDTRS.
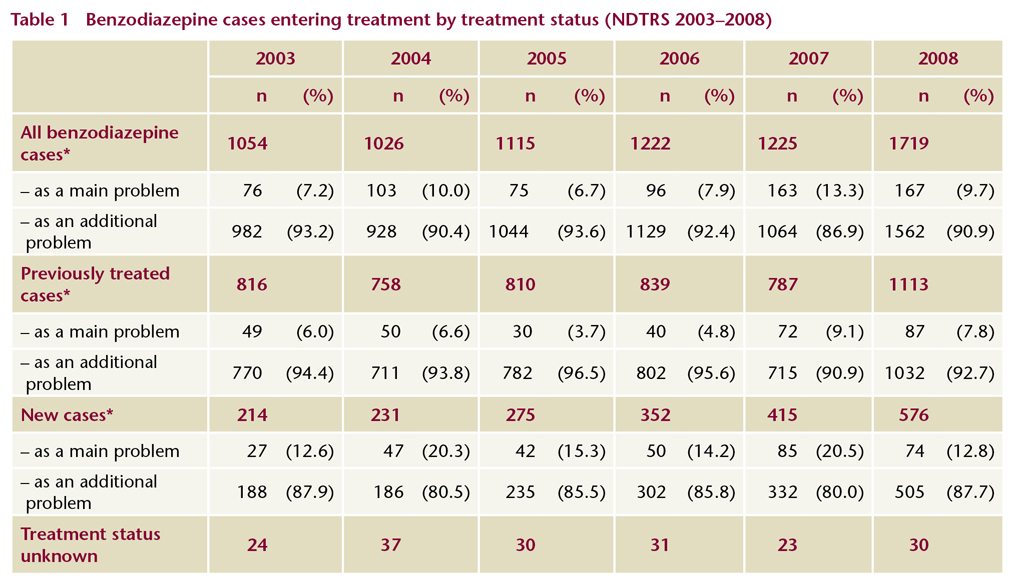
* The sum of ‘main problem’ and ‘additional problem’ cases may exceed the total number of cases in these treatment status categories as some cases reported one type of benzodiazepine as their main problem substance and another type of benzodiazepine as an additional problem substance.
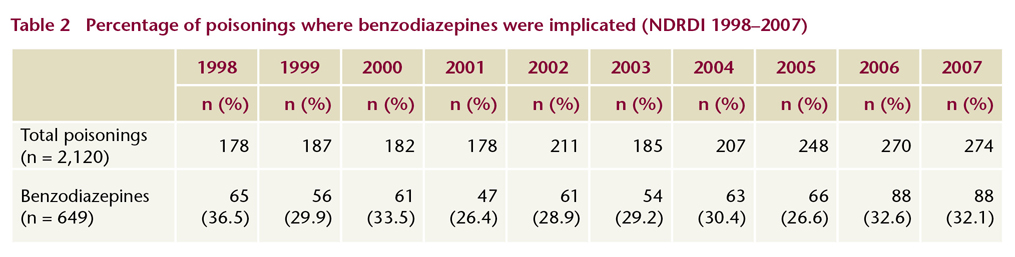
Between 1998 and 2007 benzodiazepines were implicated in 649 deaths by poisoning, which accounted for 31% of all such deaths recorded by the NDRDI for the ten-year period. The annual number of deaths in which benzodiazepines were implicated was consistently high, and increased from 65 in 1998 to 88 in 2007 (Table 2).
Substances used in conjunction with benzodiazepines
The majority (78%) of cases treated for a benzodiazepine as their main problem substance used more than one problem substance. Alcohol was the most common additional problem substance, reported by 52% of cases, followed by cannabis (43%) and opiates (40%). The main problem substances reported where a benzodiazepine was the additional problem substance were opiates (80%), alcohol (9%), cannabis (5%), and cocaine (5%). It is generally accepted that the use of several substances increases the complexity of these cases and is associated with poorer treatment outcomes. Problem use of benzodiazepines needs to be approached in the context of multiple substance use. The types of intervention and treatment setting very much depend on the individual’s current problem substances and history of substance use and on the treatment services available in the HSE area.
The additional substances most frequently involved in poisoning deaths where a benzodiazepine was implicated were alcohol (41%) and methadone (36%). Alone, these substances may not be sufficient to cause death, but it is likely that the respiratory depressant effect is amplified when these substances are taken together, increasing the risk of fatal overdose.
Age and gender
The median age of new cases entering treatment for a benzodiazepine as their main problem substance decreased from 34 to 25 years over the reporting period, while the median age of previously treated cases remained stable, ranging between 27 and 29 years. The median age of cases entering treatment and reporting a benzodiazepine as an additional problem substance increased from 24 to 26 years for new cases, and from 27 to 30 years for previously treated cases. Although the numbers were small, the proportion of cases aged under 18 years increased steadily between 2003 and 2008, and was highest among new cases who presented with a benzodiazepine as their main problem substance. This finding has implications for health promotion, drug awareness campaigns and service provision for this vulnerable age group.
The median age of those who died as a result of poisoning where a benzodiazepine was implicated ranged between 33 and 39 years over the reporting period. Just over half (51%) were not alone at the time of their death. The majority of poisonings occurred in a private dwelling.
Approximately 70% of all benzodiazepine cases treated in the period 2003–2008 were males and the proportion was the same for new cases and for previously treated cases. However, the male to female ratio differed depending on whether benzodiazepines were reported as a main or an additional problem substance. Over the six-year period, females accounted for 40% of cases with a benzodiazepine as their main problem and 30% of cases with a benzodiazepine as an additional problem substance. Among those who reported a benzodiazepine as their main problem substance and who had no history of opiate use, there were higher proportions of female cases in the older age groups and higher proportions of male cases in the younger age groups. Similarly, among those who died, there were higher proportions of females in the older age groups and higher proportions of males in the younger age groups.
Age, gender, history of opiate use and whether benzodiazepines are a main or an additional problem substance are all factors that need to be considered by services treating this population. The increasing number of cases in treatment and the number of deaths among the population support the findings of the most recent national drug prevalence survey, which showed that 11% of all adults had used sedatives or tranquillisers (which include benzodiazepines) at some point in their lives. Prescribers and users need to be made more aware of the potentially fatal effects of benzodiazepines used in conjunction with other substances. Identifying and controlling possible illicit sources of benzodiazepines is also necessary, but it is equally important to revisit the clinical guidelines on benzodiazepine prescribing.2