Dillon, Lucy (2019) Headshop legislation and changes in drug-related psychiatric admissions. Drugnet Ireland, Issue 71, Autumn 2019, p. 13.
| Preview | Title | Contact |
|---|---|---|
|
PDF (Drugnet 71)
1MB |
The impact of changes in legislation on drug-using behaviour is an area of interest for policymakers and other stakeholders. In 2017, a paper by Smyth et al. explored the relationship between changes in Ireland’s legislation related to new psychoactive substances (NPS) and their problematic use by looking at national drug treatment data.1 While acknowledging other possible explanations, the authors argued that their findings ‘are consistent with a hypothesis that the legislation and consequent closure of the headshops contributed to a reduction in NPS-related substance use disorders in Ireland’. They concluded that:
While policy responses based on prohibition type principals appear to have fallen out of favour globally in the past decade, the experience of Ireland’s response to NPS suggests that such policies remain a legitimate component of society’s response to this complex and ever-changing challenge.
A 2019 paper by Smyth et al. builds on this analysis by exploring the same research question using drug-related psychiatric admissions (DRPAs) data rather than treatment data.2
Context
As outlined in a Drugnet Ireland article on Smyth et al.’s 2017 paper, in 2010, NPS were the subject of two pieces of legislation in Ireland.3 The first (enacted in May 2010) expanded the list of substances controlled under the Misuse of Drugs Acts 1977−1984 to include over 100 NPS.4 The second, the Criminal Justice (Psychoactive Substances) Act 2010 (enacted in August 2010), differed from the established approach to drug control under Ireland’s Misuse of Drugs Act, in that it covered the sale of substances by virtue of their psychoactive properties, rather than the identity of the drug or its chemical structure. It was aimed at vendors of NPS and effectively made it an offence to sell a psychoactive substance.5 This ‘two-pronged legislative approach’ was largely in response to an increase in the number of so-called ‘headshops’ selling NPS from late 2009 to a peak of 102 premises in May 2010. By October 2010, only 10 headshops were still open and by late 2010 An Garda Síochána indicated that none of the remaining shops were selling NPS.
Legislative bans such as these have attracted international debate as to their effectiveness in impacting on the overall availability and use of NPS, in particular problematic use.6 In their 2019 paper, Smyth et al. hypothesised that ‘the expansion and subsequent abrupt closure of headshops in Ireland might cause changes to acute psychiatric presentations linked to NPS’ (p. 2).
Methods
The paper is based on analysis of data from the National Psychiatric In-Patient Reporting System (NPIRS) database, which collates data from every psychiatric inpatient unit in the Republic of Ireland. When a patient is discharged from one of these units, the clinical team identifies the primary and any additional diagnoses that led to an admission. Smyth et al. focused on DRPAs defined as either primary or any secondary discharge diagnosis that was in the F11–F19 ICD-10 diagnostic categories (International Statistical Classification of Diseases and Related Health Problems). Analysis included all DPRAs between 2008 and 2012 of people aged between 18 and 34 years. As there is no unique patient identifier in Ireland, the unit of analysis was episode of admission, not individual patient. Data are not collected on the drug used by the DRPA, so analysis is not linked specifically to NPS.
Statistical analysis was carried out to answer three core questions:
- Do DRPAs differ from other admissions in the age range 18–34? To contrast proportions, the authors used chi-squared tests, reporting odds ratios and estimates of the 95% confidence interval (CI). Twelve per cent of all admissions for the period under study (2008–2012) were DRPAs. When compared with non-drug-related admissions, DRPAs were more likely to be male, younger, have unstable accommodation, be single/divorced, and have less skilled work.
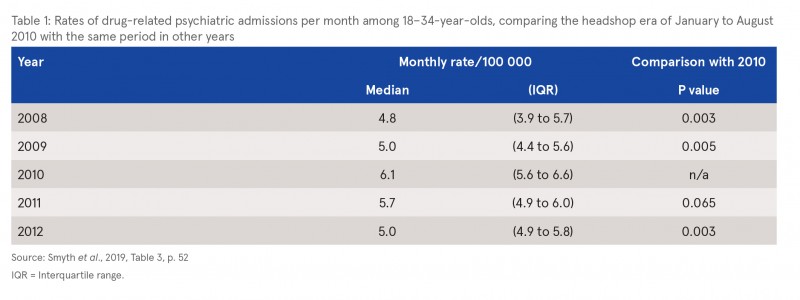
- Did the rate of DRPA increase during the ‘headshop era’ (January–August) in 2010? The authors found that the rates of admission in 2010 were significantly higher than in 2008, 2009, and 2012 (p<0.01) (see Table 1).
- Was there evidence of trend changes in DRPA and did these coincide with the arrival and departure of the headshops? The authors used the Joinpoint regression analysis that identified a significant downward trend change, which occurred in July 2010 (85% CI: Feb 2010 to April 2011). Males aged 18 to 24 years showed the greatest change, with DRPA falling by 1.4% per month (95% CI: 0.7 to 3.7% decline) from May 2010 to December 2012.
Conclusion
The authors argue that the timing of the changes found coincide with the advent of the headshop era and the subsequent introduction of legislation that essentially banned the sale of NPS in Ireland. In their discussion, the authors present these findings alongside the reduction in NPS-related treatment episodes found in their 2017 paper, and an 80% decline in NPS youth over the 4 years following 2010.7 The authors use this evidence to argue that while they recognise that correlation does not prove causation, their ‘findings lend weight to the view that the steps taken in Ireland to address NPS were associated with a positive public health impact’ (p. 7).
1 Smyth BP, Lyons S and Cullen W (2017) Decline in new psychoactive substance use disorders following legislation targeting headshops: evidence from national addiction treatment data. Drug Alcohol Rev, 36(5): 609–17. http://www.drugsandalcohol.ie/27172/
2 Smyth BP, Daly A, Elmusharaf K, McDonald C, Clarke M, Craig S, et al. (2019) Legislation targeting head shops selling new psychoactive substances and changes in drug-related psychiatric admissions: a national database study. Early Interv Psychiatry, Early online. https://www.drugsandalcohol.ie/30436/
3 Dillon L (2017) Headshop legislation and changes in national addiction treatment data. Drugnet Ireland, 62 (Summer): 13–14. https://www.drugsandalcohol.ie/27740/
4 Misuse of Drugs (Amendment) Regulations 2010. Available online at: http://www.irishstatutebook.ie/eli/2010/si/200/made/en/pdf
5 Criminal Justice (Psychoactive Substances) Act 2010 (Commencement) Order 2010. Available online at: http://www.irishstatutebook.ie/eli/2010/si/401/made/en/pdf
6 Dillon L (2016) New psychoactive substances: legislative changes in the UK. Drugnet Ireland, 59 (Autumn): 9−10. http://www.drugsandalcohol.ie/26231/
7 National Advisory Committee on Drugs and Alcohol (NACDA) (2016) Prevalence of drug use and gambling in Ireland and drug use in Northern Ireland 2014/15: Regional Drug and Alcohol Task Force (Ireland) and Health and Social Care Trust (Northern Ireland) results. Bulletin 2. Dublin: NACDA. https://www.drugsandalcohol.ie/26901/
G Health and disease > Substance related disorder > Substance related mental health disorder
MM-MO Crime and law > Substance use laws > Drug laws
MP-MR Policy, planning, economics, work and social services > Policy > Policy on substance use > Supply reduction policy
VA Geographic area > Europe > Ireland
Repository Staff Only: item control page