Long, Jean (2004) Drug situation, consequences and treatment in Irish prisons. Drugnet Ireland, Issue 12, December 2004, pp. 9-11.
| Preview | Title | Contact |
|---|---|---|
|
PDF (Drugnet Ireland, issue 12)
- Published Version
263kB |
Between 1997 and 2000, the Irish Prison Service commissioned a number of studies to examine the prevalence of blood-borne viruses 1,2 and the health status of the prison population. 3 Two independent qualitative studies were also completed. 4,5,6
In the late 1990s, two studies1,2 estimated the prevalence of antibodies to hepatitis B, hepatitis C and HIV among the prison population and described the risk factors associated with testing positive for each of these antibodies.
Among 1,193 prison inmates in 19981 the prevalence of antibodies to the hepatitis B core antigen was 9 per cent, to hepatitis C 37 per cent, and to HIV 2 per cent; two-fifths of prisoners tested positive for one or more of the infections. Of the 1,178 inmates whose injecting status was known, 43 per cent (509) had ever injected and, of these, one-fifth had started injecting in prison.
In order to adjust for the over-representation of prisoners serving longer sentences and to ensure adequate representation of prisoners held on remand or serving shorter sentences, a survey estimating the prevalence of blood-borne viruses among 596 prison entrants was completed in 1999.2 The prevalence of antibodies to hepatitis B core antigen was 6 per cent, to hepatitis C 22 per cent, and to HIV 2 per cent. One-third of the respondents had never previously been in prison (197); these had the lowest prevalence of antibodies to hepatitis B core antigen (2%), to hepatitis C virus (3%) and to HIV (0%). In total, 173 (29%) entrants reported ever injecting drugs. Only 7 per cent (14/197) of those entering prison for the first time reported ever injecting drugs, compared to 40 per cent (157/394) of those previously in prison. Of those who ever injected and had spent time in prison, 19 per cent started injecting in prison.
In the two studies,1,2 the overall pattern of injecting drug use was similar among both inmates and re-entrants. The prevalence of antibodies to all three viruses was significantly higher among both inmates and entrants who reported injecting drug use (Figures 1 and 2).
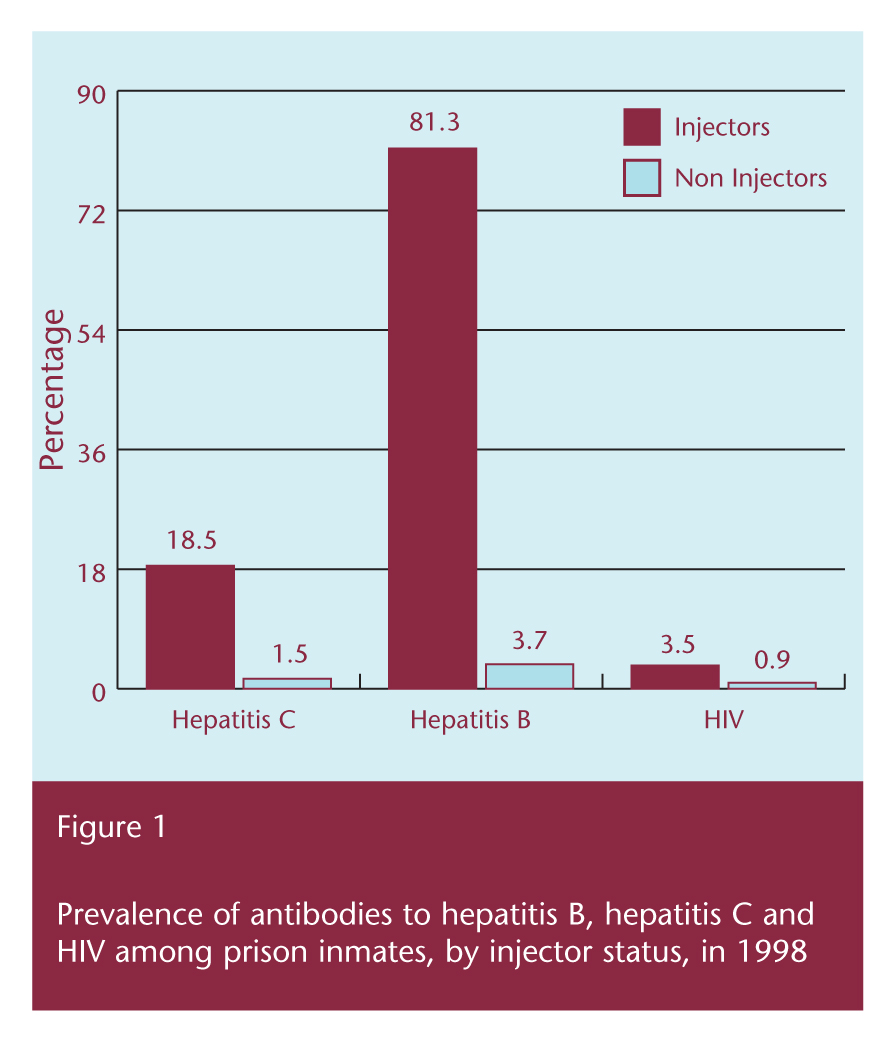
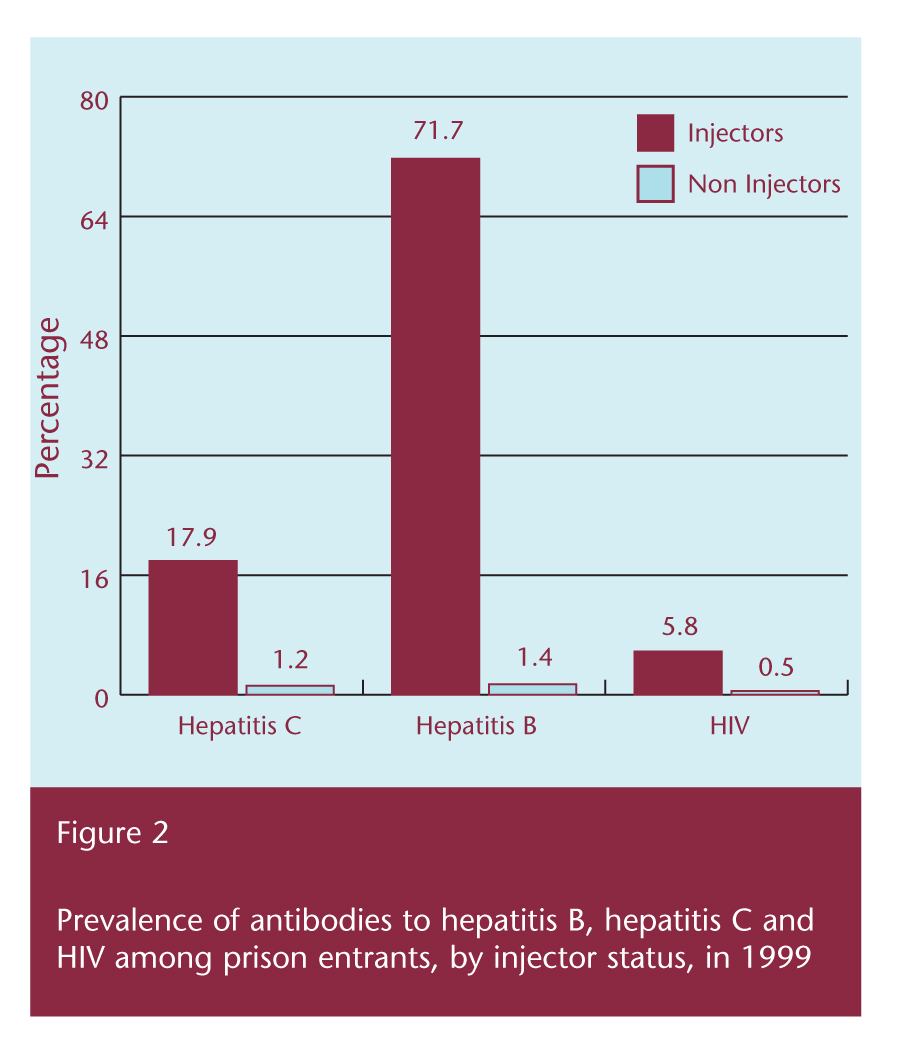
After adjusting for other risk factors in both studies, injectors who had shared needles in prison were over four times more likely to test positive for hepatitis C than injectors who had not shared needles in prison. Injectors who started injecting more than three years prior to the survey were also more likely to test positive for hepatitis C than injectors who had not injected in the month prior to the survey. Injectors who had spent more than three of the last 10 years in prison were also more likely to test positive for hepatitis C than their counterparts who had spent less than three months in prison.
The authors of the two studies concluded that hepatitis C was endemic in Irish prisons, that injecting drug use was the most important risk factor, and that being in prison would seem to increase the risk of acquiring it.
Long and colleagues described and explored injecting practices,4 strategies taken to deal with risk of infection5 and actions necessary to address this situation;4 31 participants(16 injectors and 15 non-injectors) were interviewed.
Injectors reported and non-injectors observed that ‘injectors take a number of risks during detention that they would not take outside prison’. For example, the low availability of heroin encouraged the change from smoking to injecting; the scarcity of injecting equipment meant that sharing circles were far wider than outside prison; cleaning practices were inadequate for injecting equipment, and those who owned a syringe and needle rented them to other injectors as a means of acquiring the drugs to maintain their habit. The non-injectors in prison said they knew which prisoners were current injecting drug users. Almost all non-injectors had observed injecting drug use in prison and their reported observations of injecting practices were consistent with those reported by respondents who had injected in prison.
During the in-depth interviews, prisoners (both injectors and non-injectors) were asked how they dealt with the risk of either contracting or testing positive for hepatitis C. Two dominant themes emerged: denial and fear. Injector respondents dealt with the possibility of contracting or experiencing consequences of infection with hepatitis C by: living in the moment; distancing its effects in time; generalising the condition to all injectors; and comparing its consequences to those of HIV. This process allowed them to continue injecting without considering the consequences. According to most injector respondents, hepatitis C is common among those who inject drugs and, to date, its consequences have not been serious.
The fears expressed by injectors and non-injectors were in the main well founded. Fear of contracting, or actually contracting, blood-borne viruses deterred a number of heroin users from starting or continuing to inject heroin in prison. Similar numbers of non-injector and injector respondents reported that they feared contracting blood-borne viruses while in prison.
All respondents were asked: ‘What action is required by the prison authorities to deal with drug use in prison?’ Respondents suggested a number of interventions, including routine daily activities (such as education, work, and exercise), drug awareness programmes, individual counselling sessions and harm reduction services. Non-injectors were sympathetic to the plight of injectors, and both non-injectors and injectors supported harm reduction interventions and thought that the range of drug services in prison should mirror that currently available in the community, although half opposed or had reservations about needle exchange.
Prisoners viewed time in prison as an opportunity to address substance misuse and stabilise viral infections; health professionals should not miss this opportunity.
Hannon et al. (2000) documented the health status of prisoners in Ireland, including their mental health status.3 The high rate of lifetime drug use (72% males, 83% females) occurred in a population that reported many mental health problems. In the clinical history section of this study, 30 per cent of male and 49 per cent of female respondents stated that they had spoken to a health professional about anxiety, depression or a mental, nervous or emotional problem in the past 12 months. Of these, 42 per cent of males and 58 per cent of females had sought help for depression, 13 per cent of males and 4 per cent of females for anxiety, and 14 per cent of males and 29 per cent of females for drug-related problems. Overall, 24 per cent of male prisoners and 34 per cent of female prisoners reported attending a health professional at the time of interview; of these, 17 per cent of males and 37 per cent of females were attending a psychiatrist. The association between psychiatric illness and problem drug use among prisoners was not examined in this study, but there is anecdotal evidence of a clear overlap between problem substance use and mental illness.
During 2000 and 2001 the Irish Prison Service, along with other agencies, examined the findings of these studies and developed both drug treatment service plans and healthcare plans for the prisoners.7,8 By the end of 2002, the Prison Service was at an advanced stage of drafting an Irish Prison Drug Service Policy that would be in line with the current Irish drugs strategy Building on Experience: the National Drugs Strategy 2001– 2008 (Department of Tourism Sport and Recreation 2001) and the World Health Organization’s Health in Prisons Project: Prisons, Drugs and Society 2002.9 This policy is awaiting approval from the Minister for Justice, Equality and Law Reform.
A number of positive developments have ensued, such as the introduction of evidence-based methadone treatment services that can be accessed by the majority of opiate-dependent prisoners. The Irish Prison Service is to be commended for its attempts to vaccinate a significant minority of prisoners against hepatitis B, something very few prisons, nor, indeed, community health services, have managed. The employment of registered nurses facilitated the separation of disciplinary and healthcare roles, although more needs to be done. The increased availability of drug-free units is also to be commended.
There is, of course, much more to do, such as harm reduction methods for those who continue to inject (for example, safe injecting information and limited needle exchange) and the management of morbidity (hepatitis C and sexually transmitted infections) associated with drug misuse. Counselling and psychological services are also necessary in Irish prisons and the feasibility of introducing the therapeutic community model of care for those who wish to address their substance misuse should be considered. The high levels of psychiatric co-morbidity are also worrying and indicate that a mental health strategy that is linked to the drug treatment service is urgently required.
The prison authorities and their healthcare staff have made large strides towards improving access to some drug treatment and healthcare services but, sadly, there is very little documented evidence of this because of their failure to use the existing conventional health information system; this is a missed opportunity.
1. Allwright S, Bradley F, Long J, Barry J, Thornton L and Parry JV (2000) Prevalence of antibodies to hepatitis B, hepatitis C and HIV and risk factors in Irish prisoners: results of a national cross sectional survey. British Medical Journal, 321: 78–82.
2. Long J, Allwright S, Barry J, Reaper-Reynolds S, Thornton L, Bradley F, Parry JV (2001) Prevalence of antibodies to hepatitis B, hepatitis C, and HIV and risk factors in entrants to Irish prisons: a national cross sectional survey. British Medical Journal, 323: 1209–1213.
3. Hannon F, Kelleher C, Friel S, Barry M, Harrington J, McKeown D, and McMahon A (2000) General healthcare study of the Irish prison population. Galway: National University of Ireland.
4. Long J, Allwright S, Begley C (2004) Prisoners’ views of injecting drug use and harm reduction in Irish prisons. International Journal of Drug Policy, 15: 139–149.
5. Long J, Allwright S and Begley C (2003) Fear and denial: how prisoners cope with risk of or diagnosis with hepatitis C (abstract). Irish Journal of Medical Science, 172(2) Supplement 1: 27.
6. Dillon L (2001) Drug use among prisoners: An exploratory study. Dublin: Health Research Board.
7. Irish Prison Service (2000) Report of the steering group on prison-based drug-treatment services. Dublin: Department of Justice, Equality and Law Reform.
8. Group to Review the Structure and Organisation of Prison Health Care (2001) Report of the group to review the structure and organisation of prison health care services. Dublin: Stationery Office.
9. Irish Prison Service (2003) Irish Prison Service Annual Report 2002. Dublin: Stationery Office.
J Health care, prevention, harm reduction and treatment > Health care programme, service or facility > Prison-based health service
VA Geographic area > Europe > Ireland
T Demographic characteristics > Person in prison (prisoner)
Repository Staff Only: item control page